Concept Note
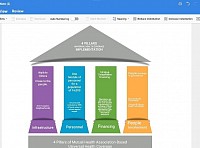
Concept Note: Our Four Pillars of Implementing Universal Health Coverage In Nigeria
Pillar 1: Health Infrastructure Within Neighbourhoods
Pillar 2: Modules of Community Health Personnel
Pillar 3: Membership Fee As Health Financing:
Pillar 4: People Involvement
Pillar 1: Primary Healthcare Infrastructure:
Open Access, Walk-In Clinics in peoples' neighbourhood across the state. The Clinics will be equipped with essential medicines and essential diagnostic point of treatment kits. The Clinics will publish daily doctors' visiting hours.
Pillar 2: Modules of hierarchical community health personnel
A Module of personnel consists of 16 Key Workers recruited and ttrained to resspond to contacts from the people about their health needs. The 16 Key Workers Task Sharing and Task Shifting 4 qualified nurses using approved Clinical Protocols supervised by a registered medical practitioner
Pillar 3: Health Financing and Health Insurance
Residents of the local neighbourhoods will have open access to the Walk-In cliniics. They will be enrolled as members of Mutual Health Associations. The membership fees of the MHA will be used as insurance premium for members.
Pillar 4: People Involvement
Mutual Health Associations will manage the Walk-In Clinics through organising membership of the association. Membership will be free for one month when free medical check up will be carried out. Thereafter, membership fees will be payable and this will be used as insurance premium for primary healthcare and ambulatory care of members.
These pillars combine Community Governed Primary Healthcare and Community Governed Health Insurance into an innovative Model to deliver Universal Health Coverage in Ekiti State, Nigeria
1. Background and Rationale
Nigeria has committed to Universal Health Coverage (UHC), yet insurance enrollment remains limited and out-of-pocket health expenditure remains high. Primary healthcare delivery is fragmented, and communities are often treated as service recipients rather than structural participants in financing and governance.
Healthcare Access Covenant Foundation (HAC) was established to translate UHC from policy aspiration into community-level implementation. Our model aligns with the mandate of the National Health Insurance Authority and global UHC principles advanced by the World Health Organization.
Ekiti State provides a viable reform environment for piloting a scalable cooperative-based primary healthcare system that integrates insurance enrollment, prepaid financing, and accountable community governance.
2. Problem Statement
Key challenges include:
Low enrollment in structured health insurance mechanisms
High out-of-pocket primary care expenditure
Limited integration of private providers into insurance networks
Weak community participation in health financing governance
Vulnerable populations excluded from prepaid systems
Without structured enrollment and local ownership, progress toward UHC remains uneven.
3. Project Goal
To establish a cooperative-based, community-governed primary healthcare network in Ekiti State that integrates insurance financing, structured service delivery, and measurable accountability systems.
4. Project Objectives (36 Months)
Establish 3–5 Community Mutual Health Association (MHA) Clinics in selected Ekiti communities, in the first year and 22 Clinics in the second year.
Enroll 5-8000 individuals per clinic into structured primary healthcare delivery and membership pre-payment insurance mechanisms.
Provide targeted contribution subsidies to 23,000–50,000 vulnerable individuals within our enrolled population, identified through a validated means-testing protocol.
Demonstrate measurable improvement in financial protection and primary care utilization.
Demonstrate sustainability of our service-insurance hybrid approach
Develop a scalable implementation framework for expansion within Southwestern Nigeria.
5. Intervention Model
Community Mutual Health Associations (MHAs)
Neighborhood-based clinics owned and governed cooperatively by members.
Services include:
Preventive annual assessments
Ambulatory primary care consultations
Essential medicines within approved protocols
Coordinated referrals
Community-based follow-up after hospital discharge
Membership Structure
Open Membership: Community registration and initial access services
Insured Membership: Annual prepaid contribution (NGN 22,500 in 2026) providing defined primary care access
Subsidy Framework
A community-validated, means-tested vulnerability assessment tool will identify individuals eligible for sponsored membership contributions. Inter-rater reliability and transparency safeguards will be built into the protocol.
6. Financing Strategy
The model operates through blended financing:
Cooperative membership contributions
Capitation payments via NHIA-aligned insurance mechanisms
Institutional grants
Targeted subsidies for vulnerable households
The objective is gradual transition toward operational sustainability by Year 3.
7. Expected Outcomes
By the end of Year 3:
*More than 10% of the population of Ekiti are enrolled in structured primary healthcare
*Increased insurance participation within target communities
*Reduced risk of catastrophic out-of-pocket primary care expenditure
*Improved utilization of preventive and ambulatory services
*Community-elected governance structures actively overseeing performance
*Contributing to Sustainable Development Goal 3 of the United Nations.
8. Monitoring & Evaluation
HAC will implement a structured Monitoring and Evaluation framework tracking:
Enrollment and retention rates
Service utilization indicators
Financial performance metrics
Member satisfaction
Comparative analysis with non-participating communities (where feasible)
Independent financial review and periodic impact reporting will be conducted.
9. Governance & Institutional Capacity
HAC operates under:
A Board of Trustees
Clinical Audit Committee
Community-elected cooperative committees
Independent financial oversight mechanisms
Conflict-of-interest and financial disclosure policies are in place.
10. Funding Request
HAC seeks an investment of USD 1.2 – 1.8 million over 36 months to support:
Establishment of 40-45 Cooperative clinics in Ekiti neighbourhoods
Digital enrollment and health records systems
Initial staffing and operational support
Vulnerable household subsidy pool
Monitoring, evaluation, and independent assessment
Detailed budget breakdown and implementation timeline are available upon request.
11. Conclusion
Healthcare Access Covenant Foundation is building a structured, cooperative, community-owned primary healthcare model designed to advance Universal Health Coverage sustainably and at scale.
This initiative represents an opportunity to move from policy commitment to measurable implementation within a replicable Nigerian context.